For many of us, wisdom teeth can become impacted and cannot be left untreated – often requiring removal.

How do I know if my Wisdom Teeth need to be removed?

Whether or not you’re experiencing pain or discomfort from your wisdom teeth, it is generally recommended to screen for potential problems early.
Wisdom tooth removal is most suitable when:
- impaction is present, or
- infection or re-infection are likely, or
- there is the chance of damage to adjacent teeth (which would be irreversible), or
- it will help avoid the need for more complicated surgery later on.
Wisdom tooth removal is generally not recommended when the position and alignment of these teeth is good, although even in these cases we will monitor closely for the presence of cavities or gum disease.
If left untreated, wisdom teeth can cause more serious problems, like dental decay or damage to nearby teeth. However, impacted wisdom teeth do not always show any symptoms, so you might not even realise you have impacted teeth.
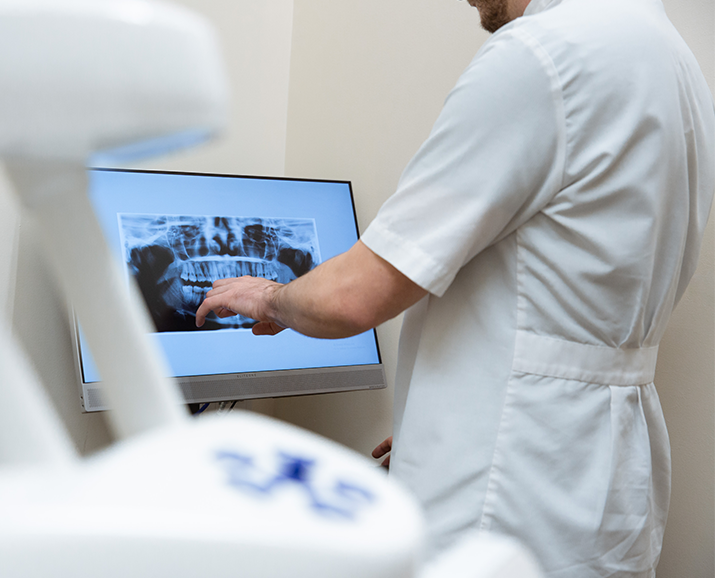
The easiest way to know if you need your wisdom teeth extracted is to visit your dentist for an examination. After your dental and medical history have been checked, you will have an X-ray to assess the position and angulation of your wisdom teeth.
When Should Wisdom Teeth be removed?

It is well documented that removal of wisdom teeth in young adults (under the age of 25) is associated with less after-operation pain and swelling than in older adults. Therefore, if it is determined that your wisdom teeth are likely to cause problems, your dentist will usually recommend that you have them removed earlier rather than later.
How to prepare for Wisdom Tooth Removal?
The length of your procedure may vary depending on how many wisdom teeth you are having removed or how complicated the removal is. Before your wisdom teeth are extracted, an anaesthetic is administered. Therefore certain precautions are warranted.
Before you undergo your extraction procedure, your clinician will outline how to prepare. You will need to fast the night before the procedure, and you should not consume alcohol for 24 hours before receiving any anaesthetic.
You will also need to organise someone to accompany you to the procedure and take you back home afterwards, and to look after you for 24 hours if your procedure has been done under sedation or general anaesthetic. We also recommend you have someone take you home if you have the procedure in-chair with local anaesthetic, but this is your choice.
What’s the procedure for treatment?
The main consideration for treatment is who should perform the procedure: a general dentist or a registered specialist?
While our general dentists can perform wisdom tooth extraction, in more complex cases we always recommend that an oral & maxillofacial surgeon carry out the procedure. These specialists are registered in the field of surgery of the mouth and jaw. In Australia they are required to qualify for degrees in dentistry, medicine and oral surgery (bringing their average training after becoming a dentist to 10–12 years).
The key benefits of seeing a specialist are to reduce the risk of temporary conditions (excessive bleeding, severe swelling, and infection), permanent conditions (damage to adjacent teeth and nerves) and post-surgical complications.
For your absolute comfort, the procedure can be performed under general anaesthetic. Medicare rebates may apply with specialist treatment.
Wisdom Teeth Removal under Local Anaesthetic
Wisdom tooth removal under local anaesthetic is done in the dental chair and renders the area to be worked completely numb. You’ll still be awake and aware of everything happening, and you may still feel pressure applied to the area.
Wisdom Teeth Removal under General Anaesthetic
When having your wisdom teeth removed using general anaesthetic, the procedure will take place in a hospital (as day surgery) and be performed by an oral & maxillofacial surgeon. A specialist anaesthetist will administer the general anaesthetic and monitor you during surgery.
Frequently Asked Questions
At Core Dental you might have your initial consultation with one of our general dentists, and then, depending on the complexity of the extraction and your personal preference, your procedure can be performed by either a general dentist or an oral & maxillofacial specialist.
General dentists can extract wisdom teeth, although many now choose to refer patients to a specialist oral surgeon. If you wish to be anaesthetised for the procedure or your extractions are expected to be more complex, it is best to be treated by a registered specialist.
Specialist oral & maxillofacial surgeons have at least 15 years’ training in both general dentistry and hospital-based surgical and medical treatments, and so have extensive experience in performing wisdom teeth extractions.
Getting specialist care for something like wisdom teeth removal is important to make sure you achieve the best possible outcome. Because they have such specialised training, oral & maxillofacial surgeons are well equipped to remove your wisdom teeth, in both simple and complex cases, and are capable of handling any complications that arise.
At Core Dental, we provide you with an itemised quotation during your consultation. This will include an estimate of any hospital and anaesthetic fees. You may then wish to contact your health insurance fund to gauge your out-of-pocket expenses.
The cost of your wisdom teeth removal procedure will vary depending on whether it is performed by a general dentist or an oral & maxillofacial surgeon.
Another factor that will affect the cost is the complexity of the removal and the type of anaesthesia used. If the surgery is performed in a hospital then there will be additional hospital fees, though Medicare and private health funds can cover some of the hospital costs.
As with all surgical procedures, there are general and specific risks associated with wisdom teeth removal, and these usually depend on whether a tooth being removed is covered by gum tissue and/or is particularly difficult to access. Your specific risks will be discussed in detail during your consultation with one of Core Dentals’ clinicians.
One uncommon complication is known as dry socket. This occurs when a blood clot has failed to form in the extracted tooth socket, or the blood clot has been dislodged. Dry socket typically occurs three or four days after the extraction. Pain (ranging from dull, to moderate to severe) and a foul mouth odour will accompany a dry socket. If you think you have developed dry socket you should contact the practice immediately for treatment.
Another possible complication, though not common, involves the lower jaw nerves being traumatised by removal of the lower wisdom teeth. This can cause an unusual sensation in the lips, tongue or gum near the treated area. Generally this complication is temporary, but in some cases it can be longer lasting. In cases where the teeth in question are close to crucial nerves, it is prudent to be treated by a specialist oral & maxillofacial surgeon to ensure a safe level of care.
A small amount of bleeding, some discomfort and a little bruising are all normal after wisdom teeth removal. The recovery time following your procedure depends on the complexity of your case; if it was a simple removal you should be back to normal the next day, but if it was more complex your recovery time could be up to a week. Pain medication can be taken to ease some of the discomfort.
When you have had your surgery at Core Dental, you will be given a post-operative pack. This will include written instructions on what to do, a medical certificate if required, additional gauzes for any post-operative bleeding, and a mouthwash and syringe for keeping the surgery site clean. We will also give you our after-hours emergency number for your peace of mind. Additionally, painkillers and antibiotics, if needed, will be prescribed.
While recovering from your surgery, you will need to maintain a soft diet (possibly just liquids) until the site has started healing. Cold foods or foods at room temperature are best. Hot food or drinks are not recommended as they can break down the blood clot in the socket and cause infection or “dry socket”. You should also make sure not to drink from a straw as this can also disturb the blood clot
After having your wisdom teeth removed it’s important to keep your mouth clean so as to prevent infection, but you will need to be careful when cleaning your teeth and be particularly gentle in the affected area.
Your clinician will instruct you on general post-operative oral care and on the following precautions:
- Avoid smoking for at least 72 hours but longer if possible.
- Don’t drink through a straw.
- Avoid dinking alcohol.
- Avoid blowing your nose.
- Avoid excessive spitting or rinsing.
- Don’t drink hot soup or other hot liquids.
- Avoid physical exertion for 24 hours.
Failure to take any of the above precautions might disturb the healing clot and cause dry socket.

